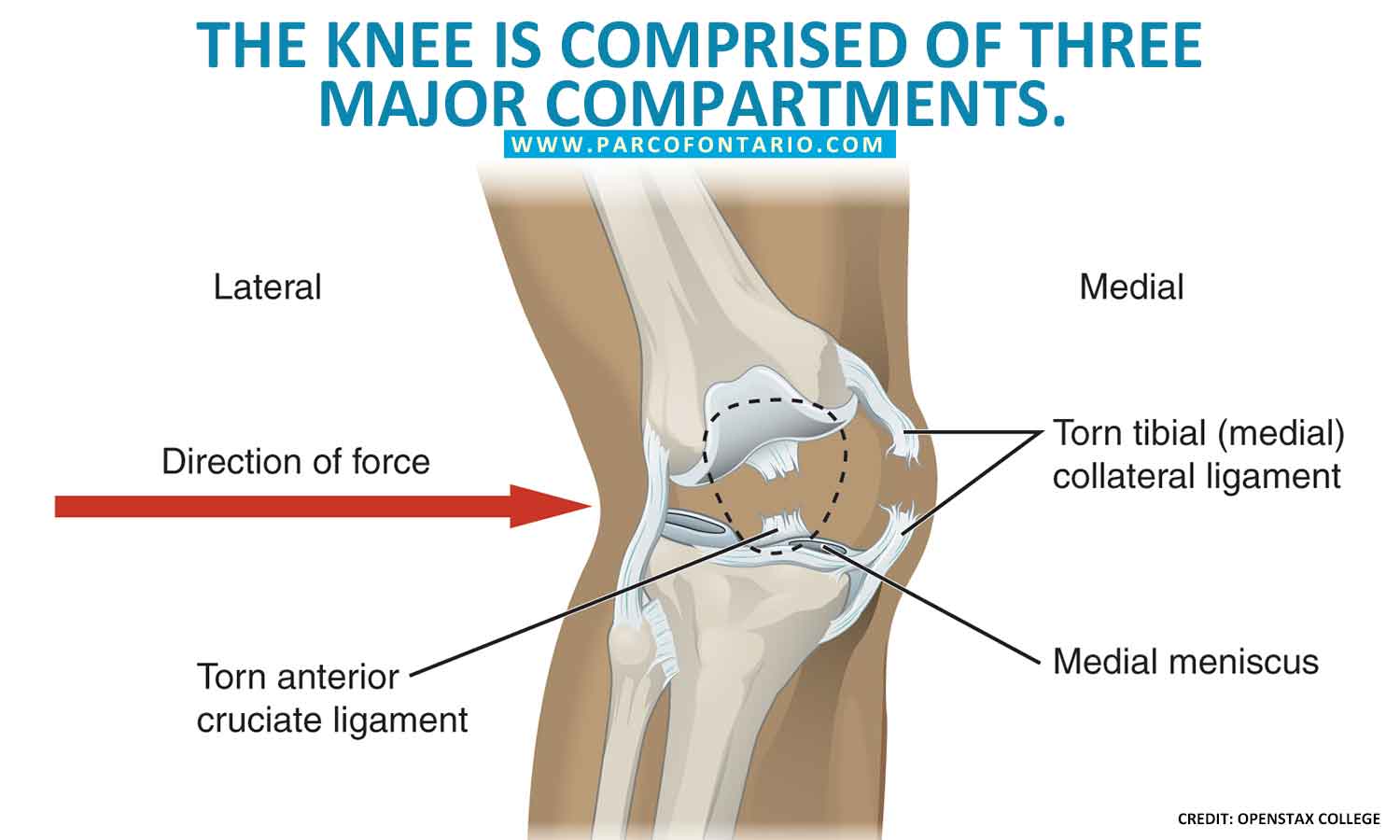
UK registry data suggests that low-volume surgeons have a higher revision rate however, the traditional contraindications of Kozinn and Scott would mean only 6% of knees are appropriate. The decision to offer patients a UKR presents a dilemma for the surgeon. 11 For this reason, UKR is contraindicated in large deformities (> 15 degrees), as they will not be corrected by the intra-articular procedure. 10 An HTO differs in that the aim of the procedure is to alter the mechanical axis of the limb. UKR will correct an intra-articular deformity caused by cartilage loss with the aim of restoring collateral ligaments to their normal tension. UKR differs from a HTO in approach to deformity correction. It must be noted that an ACL-deficient knee is predisposed to posterolateral tibial wear, which may mean a medial UKR is contraindicated as the arthritis may not be unicompartmental in nature. A UKR should be avoided if the knee is expected to be unstable after the procedure. 8 Functional instability is thought to be more prevalent in primarily ACL-deficient knees, usually resulting from trauma, compared to those with secondary ACL deficiency as a result of osteoarthritis, where the knee may still be functionally stable. 7ĪCL-deficient knees may still benefit from UKR however, the knee should be assessed for evidence of functional instability which may be considered a contraindication to a mobile bearing UKR. A medial UKR has also been shown to have excellent long-term results in patients with osteonecrosis of the medial femoral condyle. 6 The authors suggest UKR should be reserved for patients with bone-on-bone arthritis, a so called ‘kissing lesion’. The Oxford Group found that patients undergoing UKR with partial-thickness medial compartment cartilage loss on the femur, tibia or both, had poorer functional outcomes compared to full-thickness loss from both femur and tibia. 4 Patients also have higher rates of returning to sporting activities, particularly if low impact, compared to with TKR. High activity levels, once thought to be detrimental to patients undergoing UKR, have since been found to be beneficial in terms of implant survivorship and revision rates. Current criteria have suggested the consideration of UKR in situations of uni-compartmental full-thickness osteoarthritis, a functionally stable anterior cruciate ligament with stable collateral ligaments, correctable intra-articular deformity and the absence of an inflammatory aetiology. 2 It is widely accepted that these criteria are too strict and are now directly challenged in many instances.
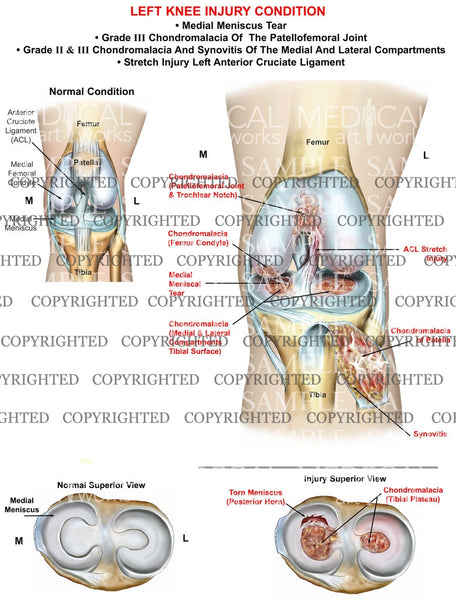
In 1989, Kozinn and Scott recommended contraindications for UKR as patient 82 kg, chondrocalcinosis, exposed bone on the patello-femoral compartment and those who are very active or undertake heavy labour. The aim of the article is to provide an up-to-date evidence base for the treatment options for such patients. In this instructional review article, we demonstrate the evidence for each option with particular focus on controversies and unanswered questions. Those who do often differ in their relative indications and contraindications to performing them. Knee surgeons differ in their willingness to offer patients such interventions. Recent research has looked into potential benefits of these options over total knee arthroplasty. 1 Recently, a trend has developed towards less invasive surgery with uni-compartmental knee replacement (UKR) and high tibial osteotomy (HTO) gaining increasing popularity. Arthroscopic debridement in the osteoarthritic knee has fallen out of favour due to poor clinical results. Traditionally, the treatment of choice would be a total knee arthroplasty however, this involves removing healthy joint surfaces. Many patients present to orthopaedic surgeons with a painful knee attributed to osteoarthritis of the medial compartment, where the lateral compartment and patella-femoral joint are relatively spared.
